Subscribe
Subscribe today to receive CGD’s latest newsletters and topic updates.
All Commentary
Filters:
Topics
Facet Toggle
Content Type
Facet Toggle
Blog Type
Facet Toggle
Time Frame
Facet Toggle
Blog Post
April 23, 2024
The ongoing global demographic transition is massive in scale and likely impact. For most of the past 200 years, the vast majority of the world’s countries have seen population growth, particularly working-age population growth. As they’ve gone through the "demographic transition" toward lower birth...
Blog Post
April 18, 2024
Achieving the UN Sustainable Development Goals (SDGs) and addressing global challenges will require a step change in private investment in emerging markets and developing economies (EMDEs). Only a small fraction of the trillions in private assets under management are currently directed to EMDEs.
Blog Post
April 17, 2024
In the wake of COVID and amidst global crises, care has increasingly become recognized as a global issue critical for sustainable development and gender equality. Yet, there are still massive gaps in care policies, services, and financing, and there is much more work that needs to happen to ensure u...
Blog Post
April 16, 2024
Last month The Gambia’s National Assembly advanced a bill that, if ratified, would make it the first country to overturn a ban on female genital mutilation. These moves—supported by the predominantly male legislature—reflect the precarious nature of gains made in gender equality and have implication...
Blog Post
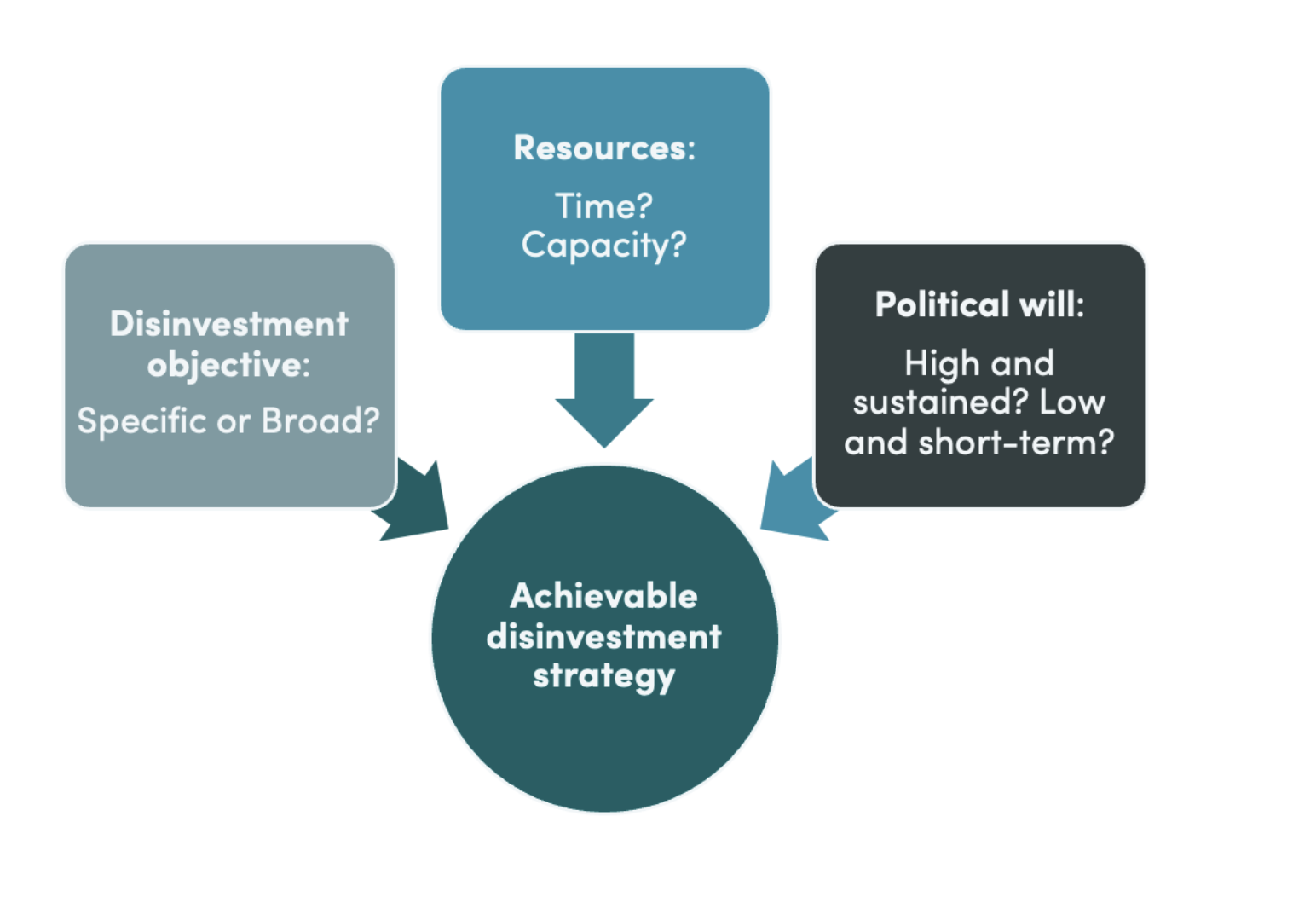
April 15, 2024
In theory, disinvestment offers the potential to release resources for achieving UHC during challenging fiscal times. However, in practice, it is time- and resource-consuming and results in less benefit than expected at the outset. The opportunity cost of launching an initiative needs to be weighed ...