This is a post with Victoria de Menil, program manager for Global Mental Health at The Stanley Center and consultant to CGD.
The theme of this year’s World Mental Health Day (Saturday, October 10th) is “dignity in mental health,” which shines light on the neglect, abuse, and inadequate treatment for the mentally ill in countries at all income levels. Globally, over a billion people are likely to experience a mental disorder in their lifetime, with the majority in low- and middle-income countries (LMIC). Mental illnesses are responsible for 7.4% of global disease burden, and frequently among the top causes of disability including in middle-income countries (Figure 1). These illnesses impose a severe economic burden not only on the individuals suffering from these illnesses but on their families, communities, healthcare systems, and governments.
Figure 1. Leading Causes of Disability in Populous Middle-Income Countries
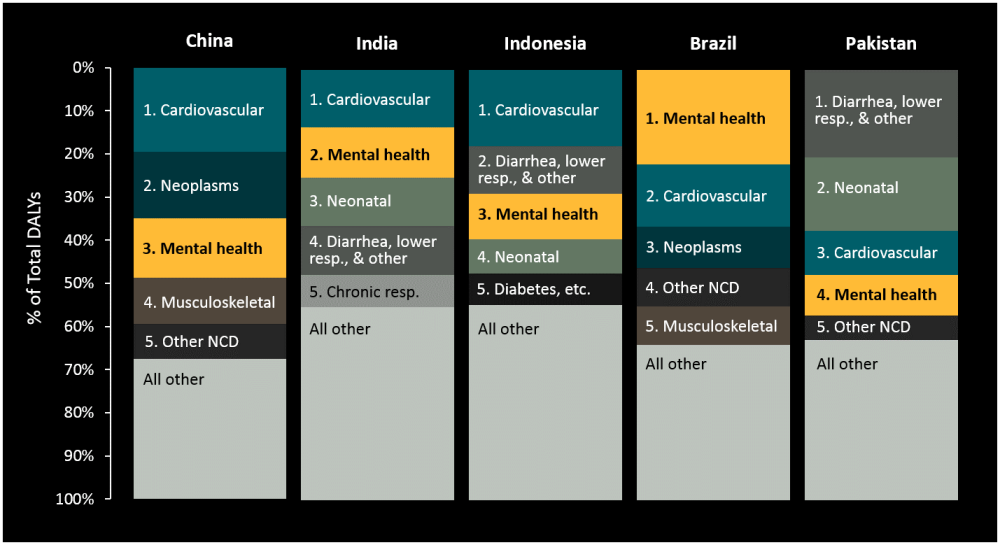
A handful of funding agencies have provided monies to mental health research and interventions in LMIC. DFID has committed £13 million towards a multi-site research consortium to improve mental health in primary care and to develop a single country’s (Ghana) mental health care system. The US National Institute for Mental Health and the Wellcome Trust have backed global mental health research initiatives for years. Grand Challenges Canada has committed $32 million to research and service delivery projects across Africa, Asia, Latin America and the Caribbean. The Open Society Foundations have supported essential work monitoring and defending human rights related to mental health care in Eastern Europe and Africa.
Despite this important support, there is still more research than action, and a yawning chasm between what we know and what we do. Less than one percent of international development assistance for health is devoted to promoting mental health or preventing or treating mental and substance-use disorders, and public spending in LMIC themselves is almost undetectable except in the form of psychiatric hospitals.
The evidence base on the cost-effectiveness of mental health interventions, and on the cascade effects of good mental health on other health outcomes, is growing in LMIC. The third edition of the Disease Control Priorities Project (DCP3)—which provides the latest evidence on the efficacy and effectiveness of interventions tackling the world’s largest disease burdens—for the first time dedicates an entire volume on mental, neurological, and substance use disorders, a testimony to the growing (though still inadequate) availability of information on what works.
Building on the DCP3 and other work, a new CGD policy paper explores three big opportunities to scale up cost-effective interventions to improve mental health, based on our own thinking as well as a private group discussion attended by experts in the field.
Our goal was to name three immediate strategies that would help with the financing and implementation of cost-effective mental health care and prevention:
1. Look closely at how mental health interventions fit into health benefits plans
Countries like India, Ethiopia, and South Africa have approached mental health coverage through new mental health policies, but lacked explicit financing to support them. Mechanisms used to prioritize interventions for financing and payment within universal health coverage (UHC) policies, such as national health benefits plans or essential medicines lists, could be a solution to this problem, as long as they are effectively used to budget, procure medicines, and commission/purchase services. Including the treatment of common mental disorders within primary care has been one of the most accessible means of achieving progress. More data is necessary, however, on the extent of mental health coverage within existing national benefits plans, and the degree of budgeting and payment associated with interventions.
2. Build on results-based funding initiatives
Results-based funding between donors and health systems in LMIC may offer an innovative approach to fund mental health programs and to finance providers within health systems, existing as an alternative and complement to other forms of financing such as a traditional development assistance for global health. Investment for mental health could come from a number of new avenues; natural synergies exist between mental health and other non-communicable diseases, as well as maternal and child health.
In fact, the relative silence but growing awareness about mental health within maternal and child health and related areas creates a prime opportunity to step in. For example, a bilateral donor could contribute to the World Bank’s Global Financing Facility in Support of Every Woman Every Child (GFF) with funding earmarked for mental health prevention and treatment. These funds could be distributed within existing RBF packages already funded in the GFF’s target countries. In this way, mental health would be mainstreamed within existing platforms of healthcare, strengthening the overall health system. Another opportunity for scaling up global mental health in the near future could be found in development impact bonds. Attention must be paid to the careful definition of the kinds of outcomes to be incentivized, of course.
3. Cash transfers
The proven effectiveness of cash transfers at overcoming demand-side barriers to accessing healthcare makes them an appealing option, despite some limitations. The opportunities for uptake in global mental health are multiple.
First, a cash transfer program could be designed specifically as a mental health intervention. Based on existing evidence, this would likely be a conditional cash transfer targeting households with specific vulnerabilities towards poor mental health (e.g., low levels of education, high levels of food insecurity). One such vulnerable group is victims of humanitarian disasters. The High Level Panel on Humanitarian Cash Transfers, convened by the British government and chaired by our colleague Owen Barder, concluded that cash transfers are a major opportunity to improve humanitarian aid.
Second, community-based mental health promotion could be incorporated within existing conditional or unconditional cash transfer programs involving health promotion interventions such as health talks. A third opportunity would be to use the targeting platform of existing cash transfer programs to reach vulnerable families and communities and connect them with mental health services. However, these ideas remain to be tested, as at present mental health is mostly absent from discussion of cash transfers.
Building on the momentum of World Mental Health Day and the new DCP3, we’re urging policymakers and global health funders to take these recommendations forward – they are practical, low-cost and potentially high-impact. We’d also like to see the recommendations reflected in upcoming discussions at the World Bank and WHO’s high-level international meeting on global mental health, to be held in April 2016.
DISCLAIMER & PERMISSIONS
CGD's publications reflect the views of the authors, drawing on prior research and experience in their areas of expertise. CGD is a nonpartisan, independent organization and does not take institutional positions. You may use and disseminate CGD's publications under these conditions.





