The online platform C19economics was created to support researchers and decision makers by collating the health economic literature published on the COVID-19 pandemic into an easily searchable repository. To do so, we screened over 13,000 resources (see our methods) and the site now includes over 665 papers covering a wide geographic base and a broad range of subject areas.
After reviewing the literature, we found three notable gaps in coverage in terms of geographical focus and topic areas.
1. There is a strong geographic bias towards a handful of high-income countries
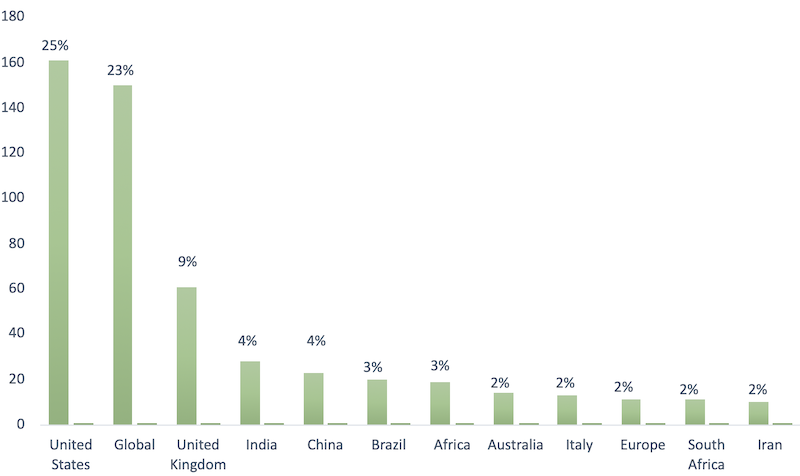
Research covering the impact of COVID-19 in the United States and the United Kingdom accounted for 25% and 9% respectively of applied country or regional research. This does not reflect a greater disease burden in these areas but appears to be driven by the greater capacity to conduct research. Following these, the most researched countries were India, China and Brazil. There is a steep drop off in the number of papers written about any country outside the top ten.
This result demonstrates that there is a need for more work to be done on ascertaining how COVID-19 is impacting other geographical areas. This is particularly true for low-and middle income- countries (LMICs) which are highly underrepresented in the literature, yet are more adversely affected. For example, Brazil was the fifth most highly covered country in the repository and experienced the high death toll of 534,233 by the end of June 2021, but it was the subject of only 21 papers. Other LMICs were the subject of only one or two publications.
Figure 1. Geographic focus
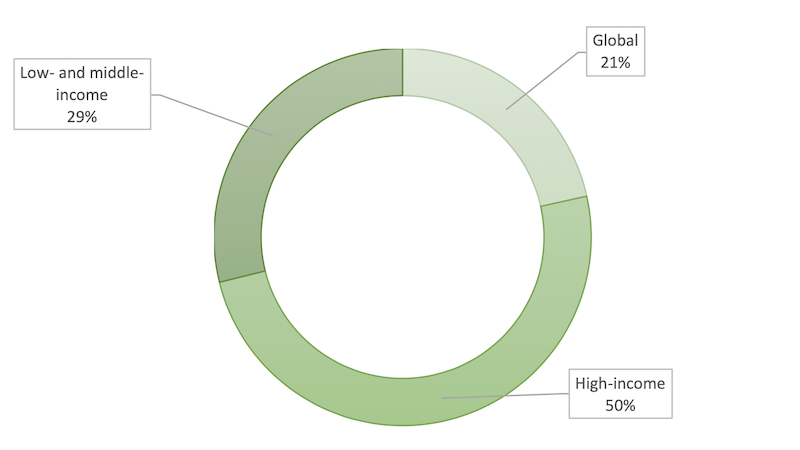
The split in the geographical focus of the coverage is even more striking when the results are grouped by income, with half of the research conducted covering high-income countries (HICs).
Only 29% of the total papers studied the effect of the pandemic on LMICs, suggesting that LMICs are highly underrepresented in the literature as a research topic.
Although 21% of papers had a global focus, this meant that the papers either grouped country level outputs for numerous countries without a particular regional focus, or had no geographical focus and were theoretical or commentary pieces. The generalisability of their results for LMICs was therefore limited in practical terms.
Figure 2. Studies by country income groups
2. Gaps in the literature appeared when the areas of interest are segmented by income
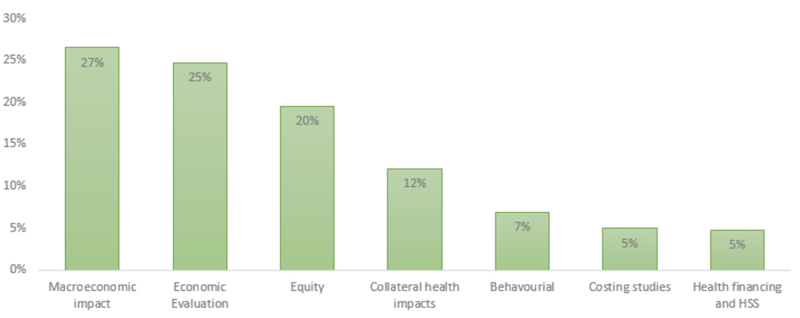
The predominant focus of the literature was found to be the macroeconomic impact of COVID-19 (27%), ascertaining the effect on different economic sectors, employment, poverty, GDP or food security. This was followed by economic evaluation papers, which included health technology assessments, cost-effectiveness analyses and estimates of budget impact. A close third were papers examining equity which involved studies looking at COVID-19 mortality or cases from a distributional perspective (gender, vulnerable, poverty, geographic, country income groups).
Figure 3. Primary area of interest
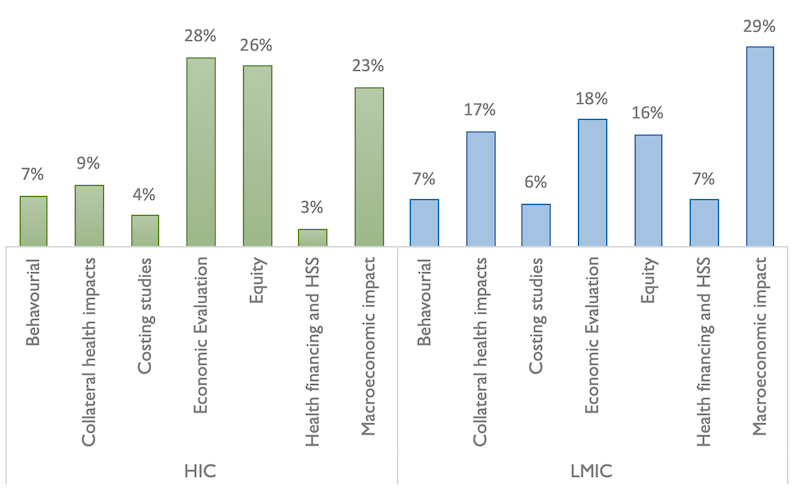
When the areas of interest were divided by income, we noted a divergence in focus. HICs had a more even spread of topics, whereas for LMICs the literature was highly dominated by studying the macroeconomic impact. The literature on economic evaluation and equity accounted for a disproportionately larger share in HICs compared to LMICs (28% vs. 18% and 26% vs. 16%). The literature for LMICs was had a greater focus on exploring collateral health impacts compared to HICs (17% vs. 9%).
Figure 4. Articles by income groups and area of interest
This is particularly important as there are limitations to using health economic evidence from different settings to inform decision making. Results may not be generalizable due to different characteristics, including epidemiology, country budgets, health systems constraints, demographics, and societal preferences.
For example, economic evaluations that modelled the benefits of a lockdown strategy balanced against business disruptions, unemployment, and the effect on the labor market would have very different trade-offs in the US compared to LMICs. The equity considerations of such policies would also differ due to the profound differences in the financial impact to the population. It is therefore crucial for more research to be published for LMICs in this area to ensure that such policies are evidence based and informed by region specific recommendations.
3. Overall there is a concerning lack of coverage of costing studies and health financing papers
Costing studies in HICs and LMICs comprised of 4% and 6% of the papers respectively. Costs are essential for establishing the economic burden of COVID-19 and it is crucial that policy development be based on informed estimates. More research producing country specific estimates could be used to provide greater illumination towards the cost impact of COVID-19 prevention measures, identify potential funding needs and can inform modelling studies.
There were similarly few results for health financing papers, although this may be a bias from our literature selection (mainly journal articles and pre-print). These are papers that considered the fiscal space, financing options for COVID-19 interventions and also looked at health systems strengthening. This is a crucial area of policy interest in order to plan a financially sustainable COVID-19 response. The pandemic has caused significant economic contractions globally which has put considerable pressure on health spending and donor aid. This is potentially devastating in resource constrained countries and may impact plans for universal health coverage. Ultimately, the pandemic has changed health systems, and diverted prioritization in funding. There is therefore a pressing need to better understand the impact of the pandemic on health system financing globally, but particularly within LMICs.
Conclusion
Overall there is a wealth of research exploring the health economics of the pandemic, however it is essential that researchers produce evidence that can be used by a wide range of countries to inform policy. We specifically call for more research to be undertaken that estimates the impact of the pandemic for low-and middle income- countries and encourage further research into costing and health financing.
DISCLAIMER & PERMISSIONS
CGD's publications reflect the views of the authors, drawing on prior research and experience in their areas of expertise. CGD is a nonpartisan, independent organization and does not take institutional positions. You may use and disseminate CGD's publications under these conditions.